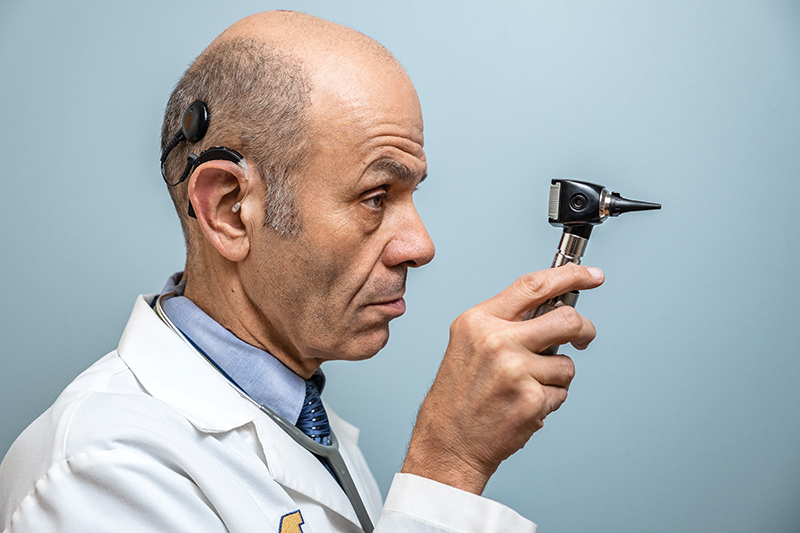
The woman drove more than an hour from a small town north of Flint to see Dr. Philip Zazove in his practice in Dexter, just west of Ann Arbor. She struggled with persistent abdominal pain, but her local doctor had failed repeatedly to help her find any relief. One session with Zazove, though, and the cause of the distress became clear: Her stomach aches were caused by anxiety and stress.
Zazove was able to diagnose her because both he and the patient are deaf. Her local physician couldn’t speak with her in her native “tongue,” American Sign Language, and thus was unable to understand her well enough to provide adequate care. “I have no idea how they communicated with her, but you can’t figure that out if you can’t talk to the patient,” he says.
To the 68-year-old Zazove, who in 1981 became only the third deaf person licensed to practice medicine in the U.S., such anecdotes underscore the life-and-death need for more doctors with a wide range of disabilities. Forty plus years later, for instance, there are perhaps 200 deaf or profoundly hard-of-hearing doctors — exponential growth but still a modest number, he says.
“It’s been proven that when a black person goes to see a doctor, they [have better health outcomes] if they have a black doctor, and a Spanish-speaking person does better if they can communicate in Spanish,” Zazove says. “The same for someone with a disability. We understand what the person is going through better.”
For the past nine years as chair of the University of Michigan Medical School’s Department of Family Medicine, Zazove has used his position to push for fundamental changes that are opening med-school educations across the U.S. to a vast new range of students with disabilities. He shepherded a landmark 2016 study that found that only one third of America’s medical schools said they would provide accommodations to students with visual, hearing, or mobility challenges. In many cases, technical standards prevent the admission of anyone who cannot hear through a stethoscope, run down a hall, or perform CPR.
“They’re not realistic,” says Zazove, who with associate Dr. Michael McKee operates the Deaf Health Clinic in Dexter. “In the real world, not everybody does CPR or runs down hallways. Most docs don’t. In most specialties — radiology, dermatology, podiatry, OB-GYN — you never do that. Some standards say you need to have the coordination to be able to draw blood. None of us draw blood. Almost none of us. They’re really excluding people who may make contributions in other ways.”
Under Zazove’s leadership, U-M itself changed its rules to permit accommodations for people like him and even has hired two doctors who use wheelchairs for the faculty, including Dr. Karin Muraszko, the chair of the neurological surgery department, who has spina bifida. He also hired Dr. Lisa Meeks, who is able-bodied but is a well-regarded expert on the subject of how to modify medical school educations to accommodate disabilities. “Michigan is very progressive,” Zazove says. “Michigan is totally becoming a leader in this area.”
Zazove is a bit of a folk hero in the world of deaf medical professionals. His 1993 memoir, When the Phone Rings, My Bed Shakes: Memoirs of a Deaf Doctor, is considered required reading for those with hearing disabilities taking an interest in health care careers. “Many deaf and hard-of-hearing students who considered medicine have read Dr. Zazove’s autobiography and realized that they too could be physicians, providing sustenance to their dreams,” says Dr. Christopher Moreland of the University of Texas at San Antonio, a 42-year-old internist who is deaf. “That’s indescribably powerful.”
Zazove has long relished exceeding expectations. That began in 1955 when, at age 4, he demanded that his father look at him when he spoke. “Why?” his father asked. “How else could you hear me?” replied the son. Young Philip had taught himself to lip-read so well that until that moment, it hadn’t dawned on anyone that he could barely hear. The cause of his loss has never been clearly identified, as is the case for many children without a family history of hearing loss. (He is almost entirely deaf, but a cochlear implant provides him with the ability to hear some rudimentary sounds.)
The 1950s were a prehistoric era for disability access, rights, education, and treatment, which is what makes Zazove’s story one of stunning perseverance and focus. His parents, both doctors, insisted that their boy be educated in mainstream classes at public schools in Skokie, Illinois, rather than segregated or sent to a school for the deaf. He mingled with the four or five other deaf children in a separated program only for speech therapy. Instead, he made stellar grades without anything other than his ability to lip-read and some modest assistance from encouraging teachers.
“There are a number of very successful deaf people and they all say the same thing — they had very supportive parents,” says Zazove as he sits in his fourth-floor office in an academic building a few blocks from U-M Hospital in Ann Arbor. “That’s the reason we make it. They told me I could do whatever I wanted, and I believed them.”
That’s not to say he didn’t encounter adversity and ignorance. In 1973, no medical school would accept him, despite his higher GPA at Northwestern University and better MCAT scores than many competing applicants. In his memoir, he groused: “I had proven myself numerous times and was tired of having to do it repeatedly. (I had not yet come to grips with the fact that I would always have to do so.) What more did they want?”
Instead, he earned a graduate degree in biology at Northwestern and applied to 35 medical schools. Just one, Rutgers, accepted him. (The New Jersey school had admitted another deaf student two years earlier: Frank Hochman, who would go on to be the second licensed deaf physician in the U.S.) Zazove ranked in the top 10% of his Rutgers class after two years but decided to transfer to Washington University in St. Louis for his last two years of medical school. There, he met a classmate who would become his wife — now-retired family practitioner Dr. Barbara Reed. Together they’d arrive in Ann Arbor in 1989 from West Jordan, Utah, to teach at the U-M Medical School and raise two daughters.
Zazove has used this perch — first as a professor and now as department chair — to advance an agenda to improve the health and lives of deaf people. In the 1990s, he was on the committee that recommended to the state of Michigan that all newborns receive hearing testing within days of their births, a change that has reduced the average age when hearing loss is detected in small children. He also became the former vice president of the Association of Medical Professionals with Hearing Losses in 2000, a group that drew about 400 attendees to its biennial conference in Baltimore in 2019.
His practice in Dexter, which includes a second deaf doctor in McKee, is a regional magnet for patients flummoxed by providers who won’t offer interpretive services. “It is akin to a hearing person in a foreign country,” says McKee, 43, an associate professor recruited to come to U-M by Zazove in 2013. “Our health is so personal and treasured that not fully feeling in control is deeply unsettling.”
Zazove’s term at the helm of U-M’s family medicine department is scheduled to end in 2022, but he believes that his efforts have become a permanent part of U-M’s med-school culture. A new initiative, MDisability, is an organized effort to promote disability education and services for medical providers and patients. “I don’t think it’s going to disappear when I retire,” Zazove says. “There are too many people involved.”
McKee is one of those.
“His experience and ability to overcome his hearing loss provides an additional benefit as a mentor to me,” McKee says of his practice partner. “There were many individuals during my years growing up who tried to discourage me from my goal of becoming a family physician. It was role models such as Dr. Zazove that helped me realize that my dream was doable.”
|
|
|












